The Tenacious P (This Week’s MMWR)
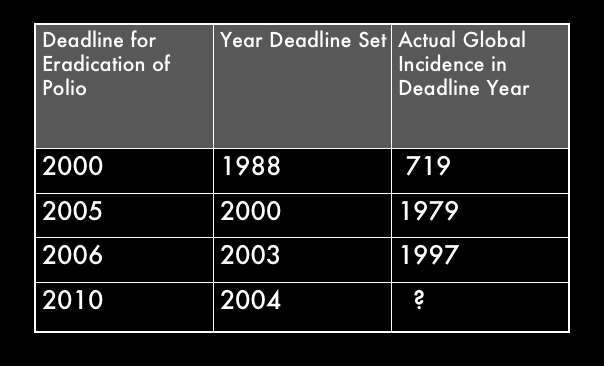
That’s P as in “polio”. This week the CDC’s MMWR reports that worldwide polio rates were pretty much flat in from 2005 to 2006, at about 2,000 cases - this despite the WHO’s Global Polio Eradication Initiative, which has set a date of 2010 for worldwide polio eradication. This 2010 date has been moved back several times, as the disease proves itself more tenacious than expected. The two-step-forward/one-step-back deadline history is rather fascinating, to me:
To be sure, there are far, far fewer cases of the disease than in the early 20th century, when it was a major worldwide killer (before Jonas Salk’s vaccine was distributed in 1962, there were as many as 58,000 cases annually - mostly among children - in the US alone). And it has been eliminated from most countries of the world; 98 percent of all global cases are now found in India, Nigeria and Pakistan. But the fact remains that it is not so easy to actually eradicate disease; that is, to vanquish it from the face of the earth. (I point here to the CDC’s definition of eradication versus elimination versus control). I’ve written about the trickiness of eradicating disease previously. The basic challenge seems to be a logistical one - even if we have the means to immunize effectively, can we ever deploy immunization so completely as to stop the disease from skipping towards a susceptible population? This is the difference, as the CDC’s report this week makes clear, between polio eradication (which we aim for) and polio control (which we pretty much have). The greater challenges here are the stuff of health metrics, and are only now starting to garner systematic and direct attention. The Gates Foundation recently helped set up an Institute of Health Metrics at the University of Washington, recruiting Christopher Murray from Harvard to take the helm. I was speaking with Dr. Murray about these sort of basic logistical challenges earlier this year, and he’s remarkably pragmatic and clear in laying out the challenges. “The more complex the treatment, the more difficult it is to implement it,” he told me, which seems self-evident until you consider how complex many of our medical treatments in fact are. Consider the further challenge of exporting those to Nigeria and the Asian subcontinent, it’s no surprise that a few thousand cases still escape our grasp.
Still, despite the statis that seems to have set in with polio eradication, there’s a hopeful section in the CDC’s discussion:
In theory if the right tools were available, all infectious diseases would be eradicable. In reality there are distinct biological features of the organisms and technical factors of dealing with them that make their potential eradicability more or less likely. Today’s categorization of a disease as not eradicable can change completely tomorrow, either because research efforts are successful in developing new and effective intervention tools or because those presumed obstructions to eradicability that seemed important in theory prove capable of being overcome in practice.
This is very intriguing to me, because it boils down to an engineering problem - a problem that I think we are very close to solving, or at least improving upon. The right tools may be just around the corner: simple-to-use DNA diagnostics that can be deployed cheaply and broadly to allow much earlier detection of polio and other infectious diseases. As D.A. Henderson, the general behind the war on smallpox, makes clear, smallpox was ideal for eradication because it the physical symptoms made it easy to detect - the pox was evident relatively early in the disease cycle, and that give health care workers a clear signal to work against. Other infectious diseases - malaria, TB, polio - don’t give off such a clear signal, at least to the naked eye. But with the right diagnostic tools, we can “see” polio and other diseases far earlier, and thus have a better chance at earlier intervention. That’s the recipe for the end of disease.


Leave a Comment